Meeting the Growing Demand for Age-Friendly Care:
A groundbreaking survey released by Age Wave and The John A. Hartford Foundation reveals widespread dissatisfaction among older adults with the U.S. health care system.
Combining results from a Harris Poll survey with focus group findings, secondary research and recommendations, Meeting the Growing Demand for Age-Friendly Care: Health Care at the Crossroads offers an urgent call from older adults for age-friendly care that meets their needs and preferences.
Watch the report release recording and access the slides.
Learn more AGE-FRIENDLY CARE.
Key Insights:
- Survey reveals wide-ranging dissatisfaction with health care and related services that don’t reflect how people want to live as they age.
- America’s 65+ population is skyrocketing as opportunities go unmet to provide better care and tailored services to enhance a person’s ‘healthspan’ versus ‘lifespan’.
- Challenges are worse for underserved communities, with dissatisfaction higher among rural residents, women and people of color.
- The movement to create age-friendly health systems can fill gaps nationwide to provide focused, high-quality care centered on the needs and preferences of older adults.
- Innovative solutions and new tech breakthroughs are beginning to emerge from both the non-profit and for-profit sectors.

Transforming Care for Older Adults
The report discusses several recommendations to improve health care for older adults and promote healthier, happier aging:
- Promote age-friendly care
- Pursue scientific breakthroughs
- Address social isolation
- Assist family caregivers
- Support a ‘national master plan for aging’
We invite the public, policy makers and health care providers to join JAHF in transforming care for older adults. Here are three ways to get involved:

Promote age-friendly care:
- Older adults can learn how to ask for and receive age-friendly care
- Health systems and clinicians can join the Age-Friendly Health Systems movement
Assist family caregivers:
- Dementia caregivers can use Best Programs for Caregiving to find support
- States, employers, funders and others can use resource guides to support caregivers
Support state and national plans for aging:
- Advocate for your state to develop a Multisector Plan on Aging
- Contribute to a National Plan on Aging currently in development
Data Highlights & Additional Recommendations
When asked to grade the overall U.S. health care system, only 11% of older adults give it an “A.” As the below selected data points show, people with more health limitations are especially dissatisfied. And while few people receive age-friendly care, those who do report higher satisfaction and better health.
Right click and “open in a new tab” to view the below charts in larger format
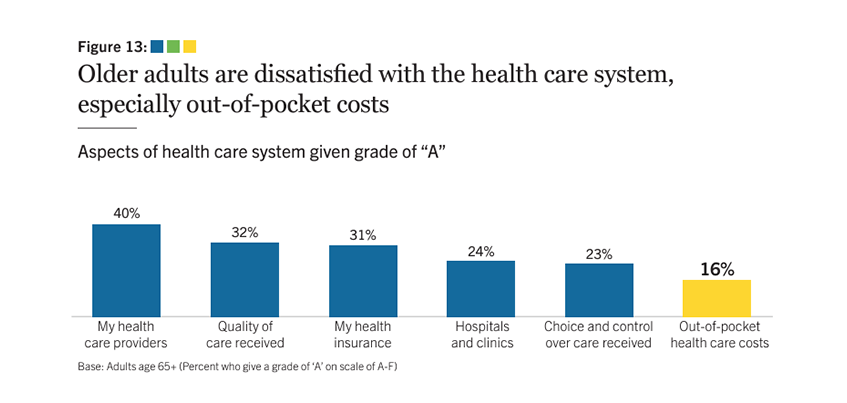
When asked to grade specific aspects of the health care system, out-of-pocket costs were rated the worst, with only 16% of older adults giving them an “A.”

Compared to other older adults, those with 3+ functional health limitations give lower grades to providers, quality of care, institutions, choice and control, and out-of-pocket costs.
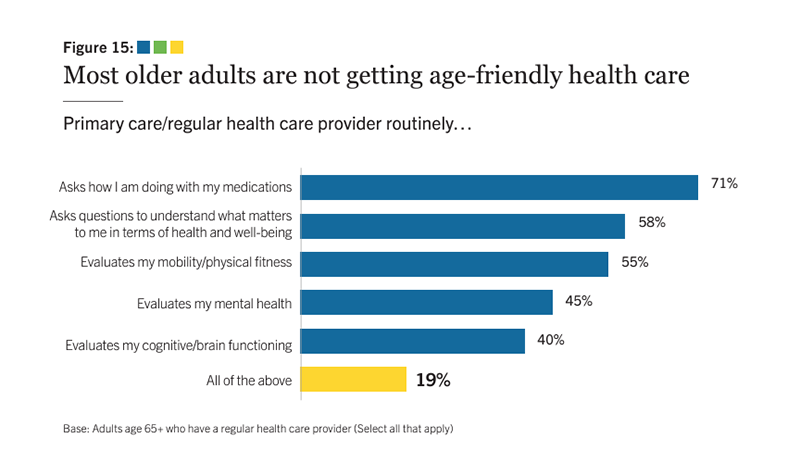
Only 19% of older adults surveyed say their health care provider routinely covers all the essentials of age-friendly care, represented by the 4Ms: what matters, medication, mentation and mobility.
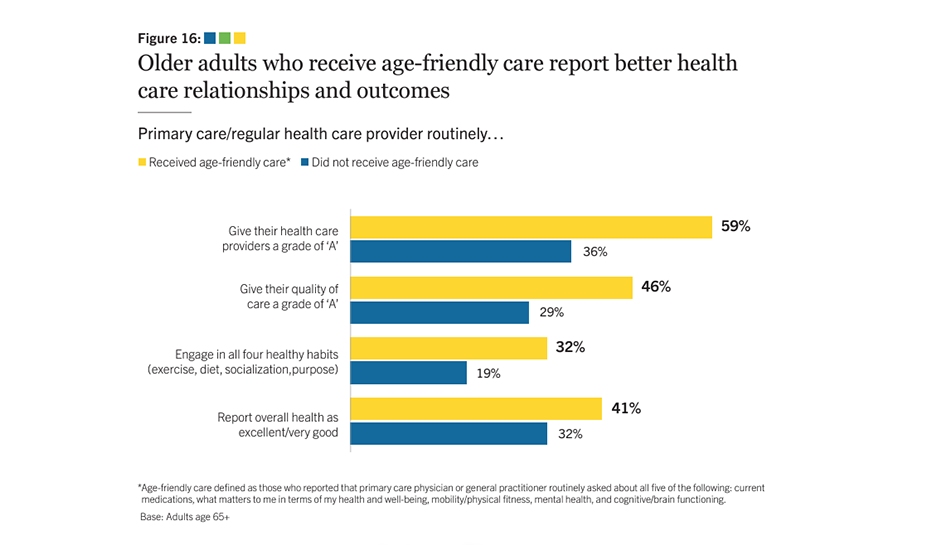
Compared to other older adults, those who receive age-friendly care give higher grades to their providers (59% vs 36%), and they report higher rates of excellent/very good health (41% to 32%).
The findings point to a set of recommendations and strategies that can better support our health and well-being as we age. Health care must become more:
Age-friendly: Safe, evidence-based health care focused on what matters to older adults. Strategy: Make basic geriatrics training and methods standard for all health care providers, using the 4Ms Framework.
Proactive: Aimed at maintaining health, function, and independence. Strategy: Redouble efforts at early detection and prevention of diseases, with the goal of increasing healthspans.
Person-centered: Empathetic and respectful care tailored to individual needs, preferences, and goals. Strategy: Scale up health-at-home, age-in-place and other programs to increase access to personalized care and functional support.
Comprehensive and Integrated: Incorporating all facets of health (including physical, mental, and cognitive) and coordinating care across providers. Strategy: Develop better AI-enabled navigation services that simplify access to care and enable older adults to better understand and manage their care.
Equitable: Removing social and financial biases and barriers that lead to current health and care-related inequities. Strategy: Lower costs to health care consumers, especially the costs of prescription drugs and long-term care, and screen for social determinants of health, such as social isolation.
Given the differences in responses to our survey based on income, geography and race/ethnicity, creating equitable age-friendly care is essential.
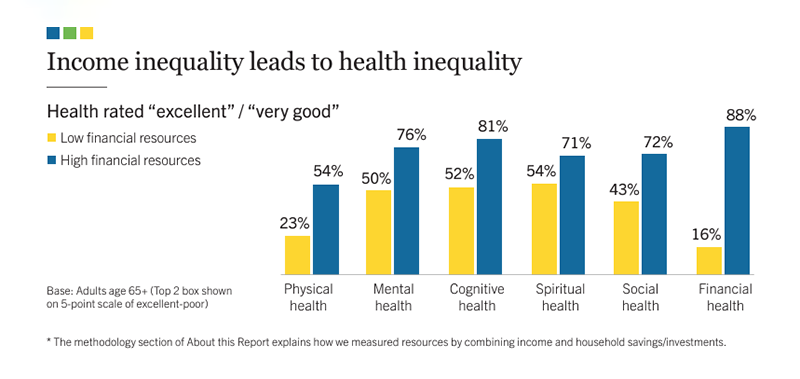
Only 23% of older adults with lower financial resources rate their physical health as excellent/very good, compared with 54% of older adults with higher financial resources.
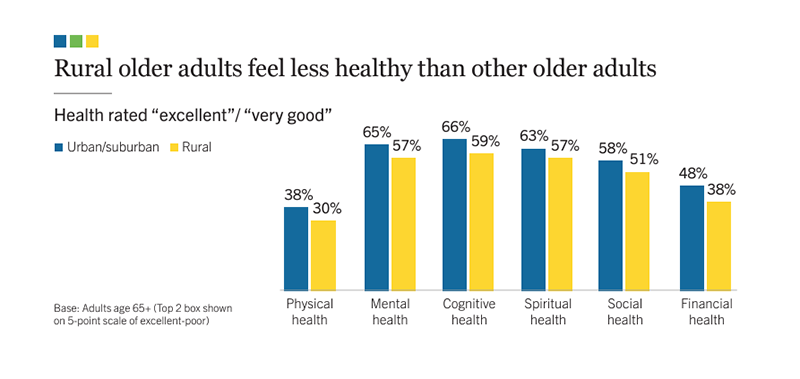
30% of rural older adults rate their physical health as excellent/very good, compared to 38% of urban/suburban older adults.
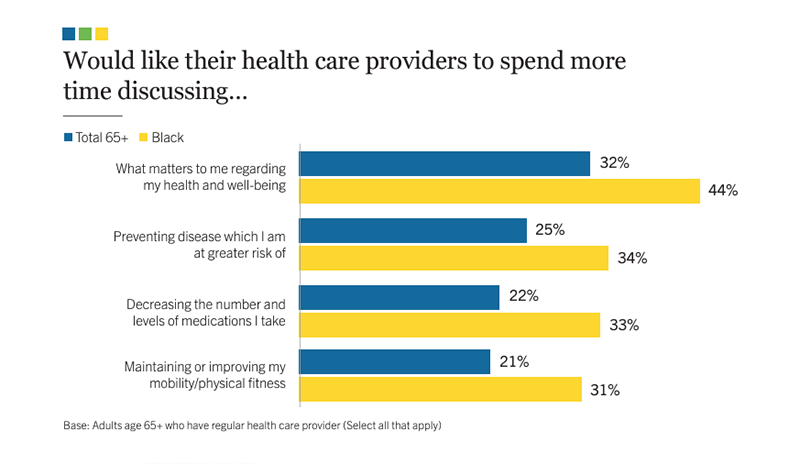
44% of Black older adults reported wanting their health care providers to spend more time discussing what matters to their health and well-being, compared to 32% of all older adults.
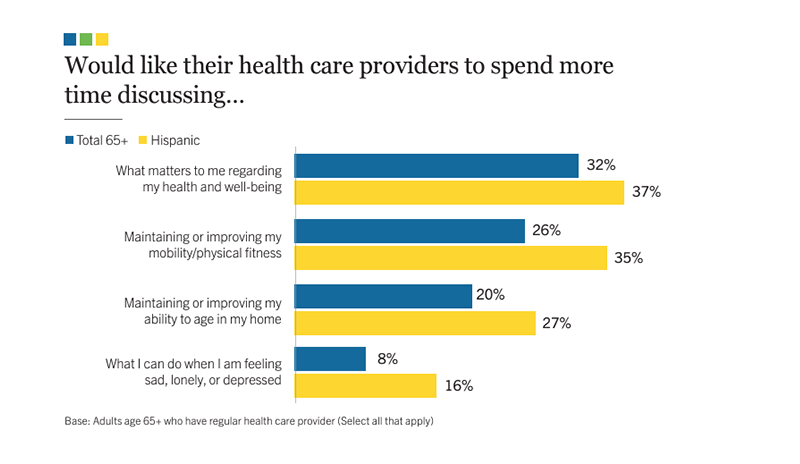
37% of Hispanic older adults reported wanting their health care providers to spend more time discussing what matters to their health and well-being, compared to 32% of all older adults.
Methodology
The study was conducted by Age Wave on behalf of The John A. Hartford Foundation and in partnership with The Harris Poll. After thorough review of secondary research, we conducted qualitative research with older adults through online focus groups, and we then conducted a nationally representative online survey. The survey was conducted April 17 to May 9, 2024. Of 5,023 adult (age 18+) respondents, 2,516 were age 65 and older. Data were weighted where necessary to align them with their actual proportions in the population, including by age, gender, race/ethnicity, region, education, household income, size of household, marital status, and political party affiliation. In order to segment respondents by financial resources (low, medium, high), The Harris Poll created an index that balances household investable assets and household income demographic questions. This approach recognizes that annual household income alone is not a sufficient metric of financial security for older adults.
Stay Informed & Connected
Join JAHF in creating a health care system where every older adult can receive age-friendly care:
